How TMS Treatment Helps Patients Stay Consistent With Mental Health Care
Staying consistent with mental health care can feel harder than starting it. Many people begin treatment with hope, only to struggle with follow-through weeks or months later. Missed appointments, medication fatigue, side effects, and emotional burnout often interrupt progress. Transcranial Magnetic Stimulation, commonly called TMS treatment, has changed this pattern for many patients. Beyond symptom relief, TMS helps people stay engaged, motivated, and consistent with their mental health care plan.
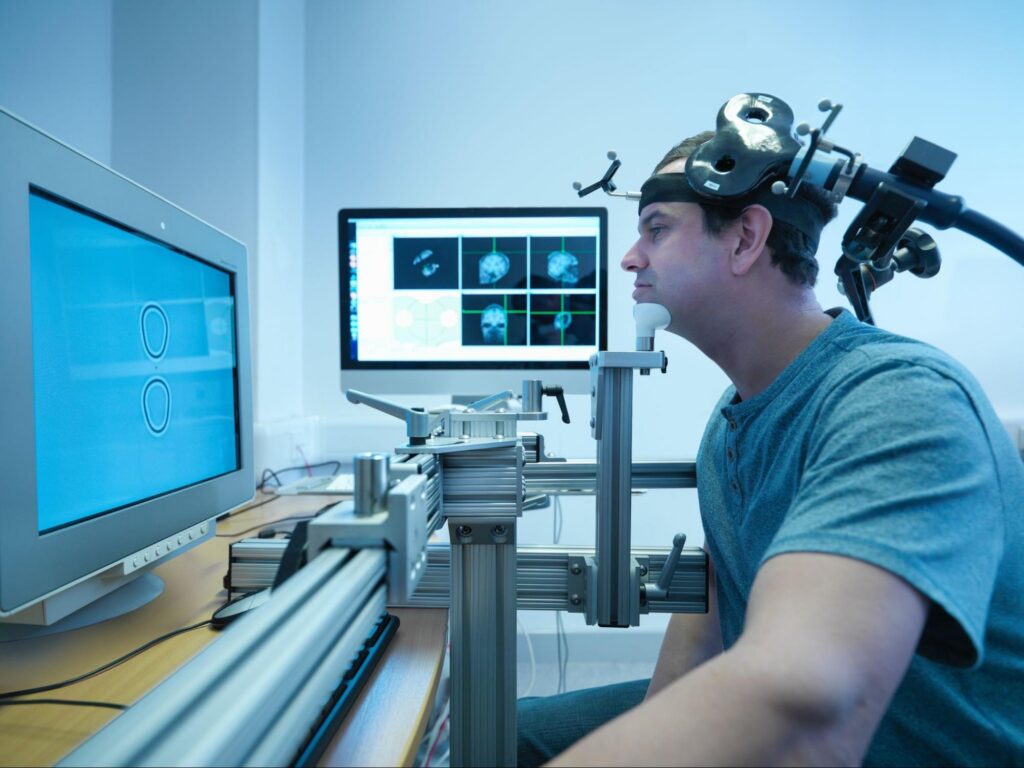
At Prime Behavioral Health in Southlake, TX, consistency stands at the center of long-term recovery. TMS treatment supports that goal in ways traditional approaches often cannot.
Why Consistency Matters in Mental Health Treatment
Mental health improvement rarely happens all at once. Progress builds through steady care, ongoing monitoring, and small adjustments over time. Inconsistent treatment often leads to symptom return, frustration, and loss of trust in the process. Missed care also makes it harder for providers to understand what truly works.
Consistency allows the brain time to adapt, stabilize, and form healthier patterns. TMS supports this process by offering structure, predictability, and measurable progress. Patients who stay engaged often report better emotional balance, clearer thinking, and stronger confidence in their care plan.
How TMS Treatment Creates a Structured Routine
One of the most powerful benefits of TMS lies in its schedule. Treatment follows a set routine, usually five sessions per week over several weeks. This structure builds consistency naturally.
Patients know what to expect, when sessions occur, and how long treatment lasts. This routine reduces uncertainty, which often fuels anxiety or avoidance. A predictable schedule helps patients plan their days, work responsibilities, and family time around care instead of skipping it.
Over time, showing up becomes a habit rather than an effort. That habit often carries over into therapy visits, follow-up appointments, and self-care routines.
Reducing Barriers That Cause People to Quit Treatment
Many people stop mental health care because of barriers, not a lack of motivation. Side effects, long medication adjustments, or feeling emotionally flat often push patients away from treatment.
TMS treatment removes several of these barriers:
- No daily medication burden
- No systemic side effects like weight changes or sedation for most patients
- No disruption to work or daily activities
- Short session times that fit into busy schedules
Removing these obstacles makes it easier to stay engaged. Patients often feel relief knowing treatment will not interfere with their identity, productivity, or daily rhythm.
Faster Symptom Relief Builds Momentum
Slow progress often leads to discouragement. People may wonder whether treatment works at all, leading to missed appointments or complete withdrawal from care.
TMS treatment often produces noticeable changes during the treatment course. Improved mood, better sleep, clearer focus, and increased motivation help patients feel the value of consistency. That momentum matters.
Once patients notice improvement, they want to protect it. This mindset strengthens commitment to appointments, follow-ups, and long-term mental health planning.
Supporting Patients Who Struggle With Motivation
Depression and related conditions affect motivation itself. Expecting someone with low energy, low hope, or emotional numbness to manage complex care plans often feels unrealistic.
TMS helps by working directly on the brain areas linked to motivation, mood regulation, and decision-making. As these areas respond, patients often report:
- Increased ability to follow schedules
- Less avoidance of appointments
- Improved emotional engagement
- Stronger sense of purpose in treatment
This shift allows patients to participate in care rather than feeling dragged through it.
Strengthening the Relationship With Mental Health Providers
Consistency improves communication. Regular TMS sessions create frequent contact between patients and care teams. These interactions build trust, comfort, and openness.
Patients feel seen and supported, not judged or rushed. Providers gain clearer insight into mood changes, behavior patterns, and emotional responses. This ongoing connection makes it easier for patients to discuss concerns, ask questions, and stay engaged.
At Prime Behavioral Health, TMS treatment integrates closely with psychiatric follow-ups and therapy, creating a coordinated care experience rather than fragmented visits.
Encouraging Long-Term Engagement After Treatment Ends
TMS treatment does not end mental health care. Instead, it often strengthens long-term engagement.
Patients who complete TMS tend to approach follow-up care with more confidence. They understand the value of consistency because they experienced it firsthand. Many continue regular psychiatric visits, therapy sessions, and wellness check-ins after treatment ends.
This continuity supports sustained improvement and reduces the risk of relapse. Patients feel empowered rather than dependent, informed rather than uncertain.
Helping Patients Regain Control Over Their Care
Feeling powerless often leads people to disengage from mental health treatment. TMS shifts that experience. Patients remain awake, alert, and active during sessions. They can work, drive, and maintain daily routines. This sense of control reinforces ownership of the recovery process.
Rather than feeling like treatment happens to them, patients feel involved in each step. That involvement strengthens consistency and long-term commitment.
Why TMS Fits Modern Lifestyles
Busy schedules, work demands, and family responsibilities often compete with mental health care. TMS treatment fits into real life. Sessions typically last under 30 minutes. Patients can return to work or daily activities immediately afterward. This flexibility removes the need to choose between care and responsibilities. Consistency becomes realistic rather than overwhelming.
Common Challenges TMS Helps Address for Patients in Southlake
Patients in Southlake and surrounding areas often face similar barriers before starting TMS. These include:
- Difficulty sticking with long-term medication plans
- Missed appointments due to fatigue or low motivation
- Frustration from slow or unclear progress
- Fear of side effects interfering with work or family life
- Emotional burnout from repeated treatment changes
TMS treatment addresses these challenges by simplifying care and supporting steady engagement.
FAQs
Does TMS treatment require strict attendance?
Yes. Consistent attendance helps the brain respond more effectively and supports better outcomes.
Can TMS help people who stopped other treatments before?
Many patients who struggled with consistency find TMS easier to maintain due to its structure and tolerability.
Will I need ongoing care after TMS treatment?
Most patients continue with follow-up psychiatric care or therapy to support long-term mental wellness.
How soon do people notice changes during TMS?
Some patients notice changes within a few weeks, while others experience gradual improvement throughout treatment.
Does TMS replace therapy or medication?
TMS often works alongside other treatments. Your provider will guide the best plan based on individual needs.
Stay consistent with your mental health care through TMS treatment at Prime Behavioral Health. Call 817-778-8884 to schedule a consultation in Southlake, TX.
